I serve clients birthing primarily in Duval County, Jacksonville Beaches and St. John’s County.
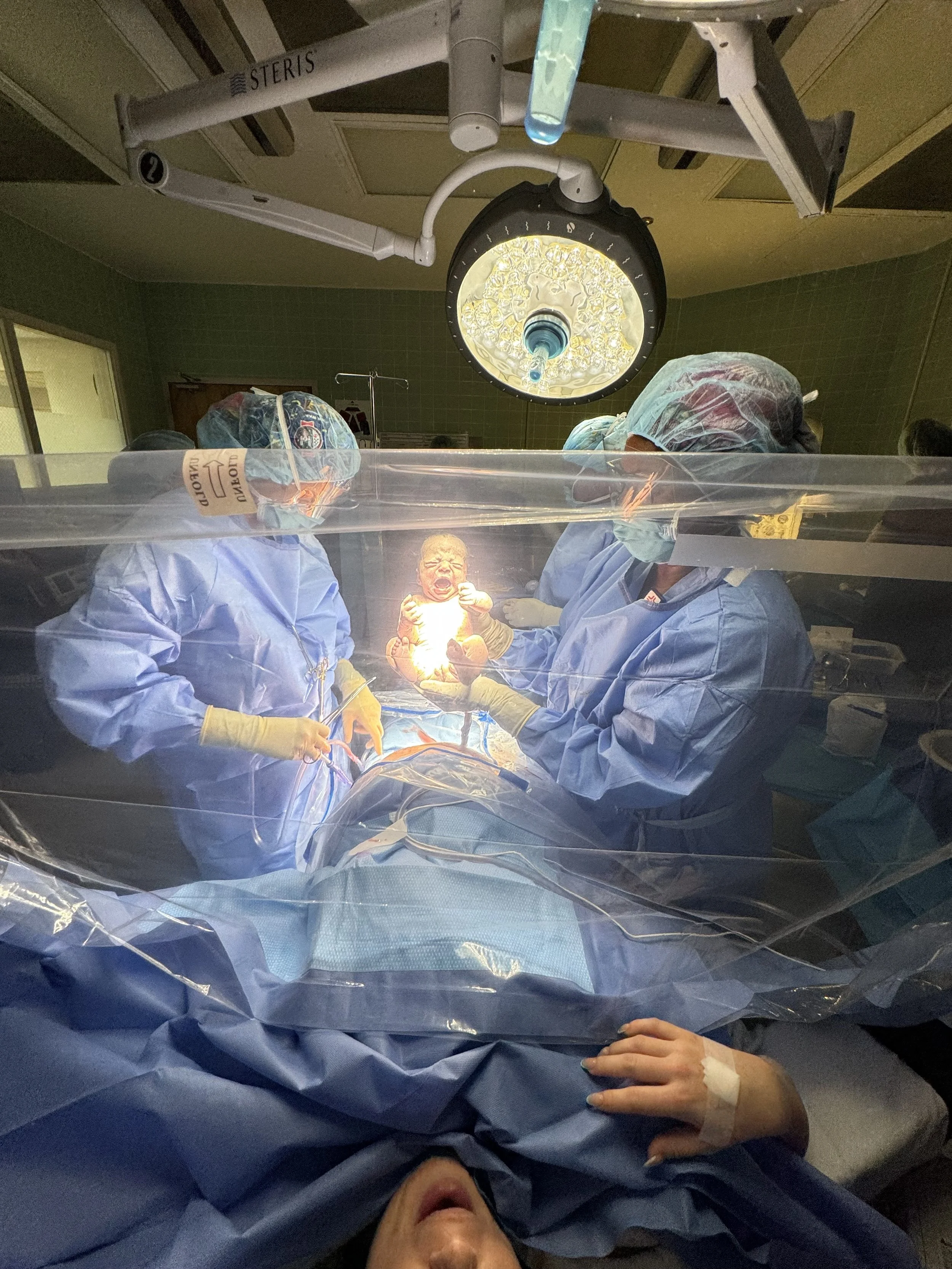
I attend births at hospitals including, but not limited to: Baptist Beaches, HCA Memorial, Ascension St. Vincent’s Southside, UF Health Flagler, UF Health North, Baptist South, Baptist Medical Center.
I support clients at all birth centers, and attend homebirths in Riverside, San Marco, Murray Hill, Avondale, Springfield, Southside, Mandarin, Orange Park, Atlantic Beach, Rivertown, Neptune Beach, Jacksonville Beach, Mayport, Arlington, Julington Creek, Mandarin, Orange Park, Nocatee, World Golf Village, Ponte Vedra, Jax Beach, and St. Augustine, among others.
I offer travel doula services to Los Angeles, parts of the East Coast, Miami-Dade, Boca Raton, Palm Beach & throughout Florida.
I’m honored to provide inclusive support to all cultures, backgrounds, spiritual and religious beliefs, medical choices, family arrangements and structures. LGBTQ+ parents are welcome here.